Sleep studies are a powerful combination of timeless human sleep knowledge and cutting-edge technology. They can extract hundreds of data points about how dozens of bodily functions are interacting with one another.
If you’re dealing with known or unknown changes in your sleep patterns and struggling to sleep better, you’re one of the most likely people to benefit from a sleep study. Learn all about sleep studies here including how much they cost and how soon you can expect results from them.
What Is a Sleep Study?
A sleep study is a comprehensive, overnight medical examination in which a sleep specialist or doctor monitors your mind and body’s sleep behavior. Most sleep studies take place at a hospital or dedicated sleep center, though some are conducted in the patient’s home.
The purpose of a sleep study is to gather data from an individual’s current sleep patterns to better understand what’s happening. Individuals dealing with issues like insomnia, narcolepsy, interruptions resulting from sleeping with a pet, and frequent movement often benefit from sleep studies.
In order to be prepared for a sleep study, you must be partially sleep-deprived. A sleep study can only be effective if you, the patient, are sleeping while it’s happening. For this reason, many sleep studies often start between 10:30pm and 11pm and may run until 6:00am or 7:00am.
When a sleep study is taking place, the doctor or specialist is observing the patient while one or more machines are collecting data. This allows for a blend of quantitative and qualitative data that’s crucial for making an informed recommendation to the patient.
There are several bodily and brain functions that a sleep study can measure, including:
- Blood oxygen levels
- Body movements (learn more about what your body does when you sleep)
- Snoring and sleep talking frequency
- Heart rate
- Breathing rate and oxygenation
- Eye movements including rapid eye movement (REM)
What Happens During a Sleep Study?
There are several things taking place during a sleep study–some based on technology and others based on human observation. Lots of data must be collected over a period of multiple hours in order to have the most accurate results and insights.
One of the first steps is connecting an electroencephalogram (EEG) to the patient’s head. An EEG has small electrodes covered by soft rubber suction cups that feed brain activity data to the machine. They’re comfortable to wear and have plenty of leeway so they don’t disrupt the patient’s sleep.
The second step often includes attaching elastic belts connected to additional machinery that measures the patient’s breathing and heart rates. These electrocardiograms and related machines enrich the data coming from the EEG and may also uncover information that another machine could not.
Doctors and sleep specialists gain hundreds of pages of data from just one sleep study, with several patterns identified from the get-go. They use these data to develop a personalized sleep treatment plan and refer back to their reports’ details if needed.
Sleep study patients can expect to receive results and personalized recommendations from their doctor about two weeks after the study. A doctor’s recommendations can be implemented quickly and patients may start seeing health improvements within the same month.
How Much Does a Sleep Study Cost?
The typical cost of a sleep study depends on whether you’re using health insurance for it or paying out-of-pocket. However, the national average price for a professional sleep study is anywhere from $2,900 to $3,000.
If you’re taking the health insurance route, depending on how much of your deductible you’ve paid, you may not pay much. If you’re paying entirely by yourself, costs can range anywhere from $1,000 to $7,000.
This may seem like a lot, but it’s actually quite normal. Expenses that go into this price range include the doctor’s salary, machinery use and upkeep costs, utility fees, material replacement costs, and analysis and delivery of results.
Given how expensive professional tests can be, consumers are turning to home-based sleep studies in greater numbers. While at-home sleep tests can’t provide the same clarity and depth that medically-administered sleep studies do, they’re a good backup option to have.
What Conditions are Sleep Studies Useful for Diagnosing?
Sleep studies are useful for diagnosing a range of sleep disorders, including sleep apnea, narcolepsy, periodic limb movement disorder (PLMD), insomnia, restless leg syndrome (RLS), excessive snoring, and sleep walking/talking.
A sleep study is an effective treatment approach for such issues for two reasons. One, specific disorders can’t be authoritatively confirmed without the input of a licensed medical or sleep health professional. Two, once the cause of the issue is determined, it’s much easier to develop a personalized treatment plan.
What are the Different Types of Sleep Studies?
Sleep studies in general are powerful, but what’s even more fascinating is the fact that there are multiple types of sleep studies. Here are the main four to know about and the details that differentiate them:
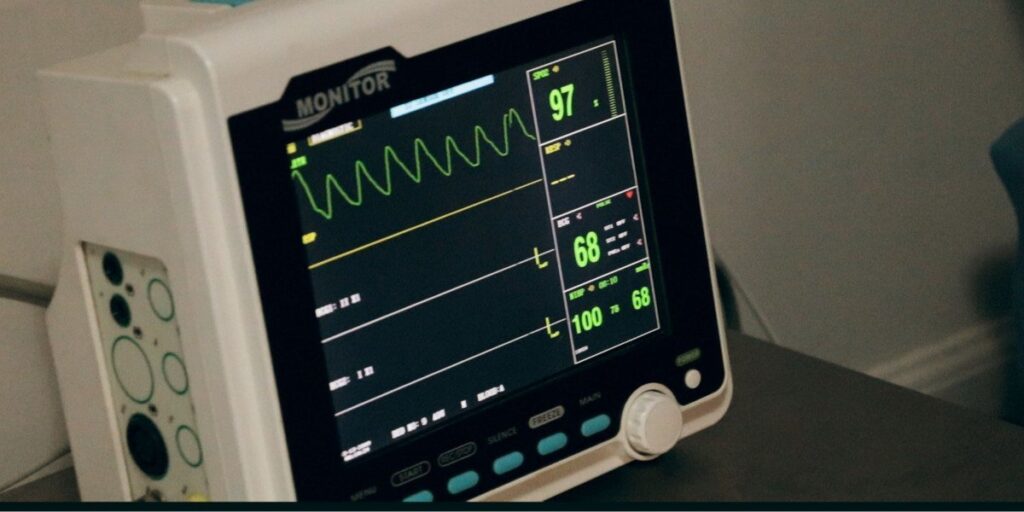
- Polysomnographic test. This is a fancy word that basically means “multiple data sources about your sleep.” Polysomnography is the most common type of sleep study and is the test utilized at most sleep centers and hospitals. Heart rate, airflow, brain activity, and muscle and eye movements are the main components measured.
- CPAP titration test. Sleep apnea is a common sleep health disorder and can be better treated with a CAPA titration test. CPAP stands for continuous positive airway pressure and is the same name of a machine that provides air pressure for sleep apnea sufferers while sleeping. There are two stages to a full CPAP titration test: the polysomnography stage where baseline data is collected, and the CPAP titration test where the doctor determines how much air pressure is needed.
- Home-based sleep test. A home-based sleep study is the most convenient but least data-driven type of test. This setup allows individuals who are unable or unwilling to go into a hospital the opportunity to gather more information about their sleep habits. At-home sleep studies are limited by nature and can’t offer the same results or insights that a proctored test does. For this reason, at-home sleep tests are recommended only for the infirm or those who have secondary health conditions.
- Multiple sleep latency test. This type of sleep study measures how quickly the patient falls asleep and how rapidly they enter an REM phase during daytime sleep. An MSLT test is usually associated with narcolepsy treatment or another similar sleep health condition. If you know how much sleep you should get and you aren’t getting it regularly, this test may be right for you.
Home Sleep Study Equipment
If you or a family member has decided to do a home-based sleep study, you need the right equipment to get useful information out of it. You have two options: ordering an all-inclusive kit or purchasing compatible items separately.
Here’s the home sleep study equipment to obtain before you start collecting data:
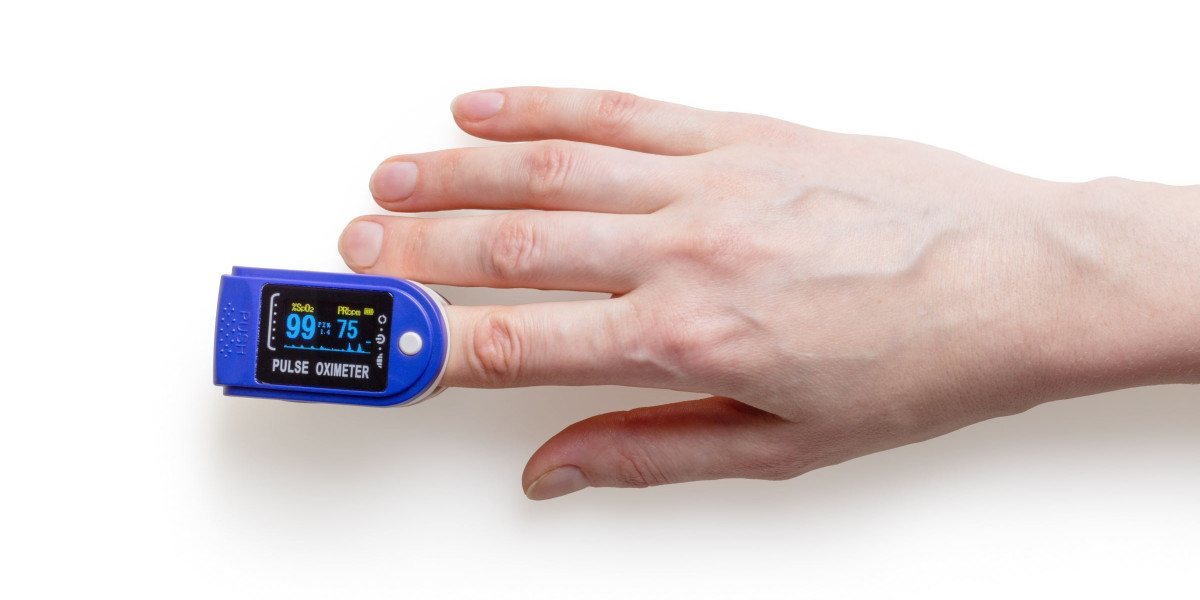
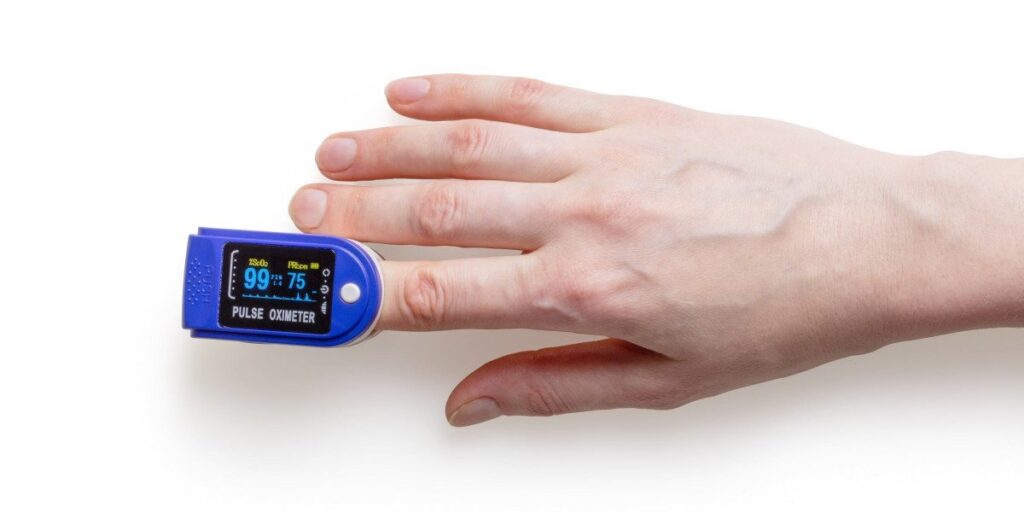
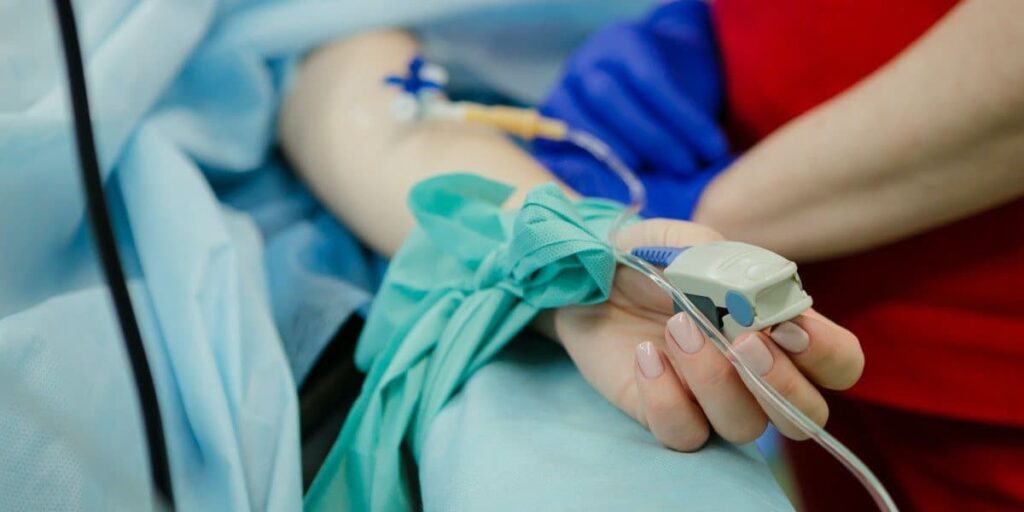
- A pulse oximeter. Pulse oximeters are small, comfortable fingertip devices that automatically measure your level of blood oxygenation. A blood oxygen level anywhere between 95 to 100% is considered normal and healthy, whereas anything below 90 to 88% is a red flag.
- A breathing sensor. This is a silicone device that’s placed in the sleeper’s nostrils and secured behind the ears with a comfortable strap. Breathing sensors measure both inhaled and exhaled air pressure as well as the sleeper’s breathing regularity.
- A breath effort belt. Breath effort belts, often shortened to just effort belts, are placed around the abdomen. This device measures the muscle and bodily movements associated with breathing and is useful in uncovering any unexpected respiratory blockages or deficiencies.
- A peripheral arterial tonometry watch. This device measures your blood flow whenever a lapse in breathing occurs. PAT watches are extra useful for those facing potential narcolepsy, sleep apnea, or severe snoring.
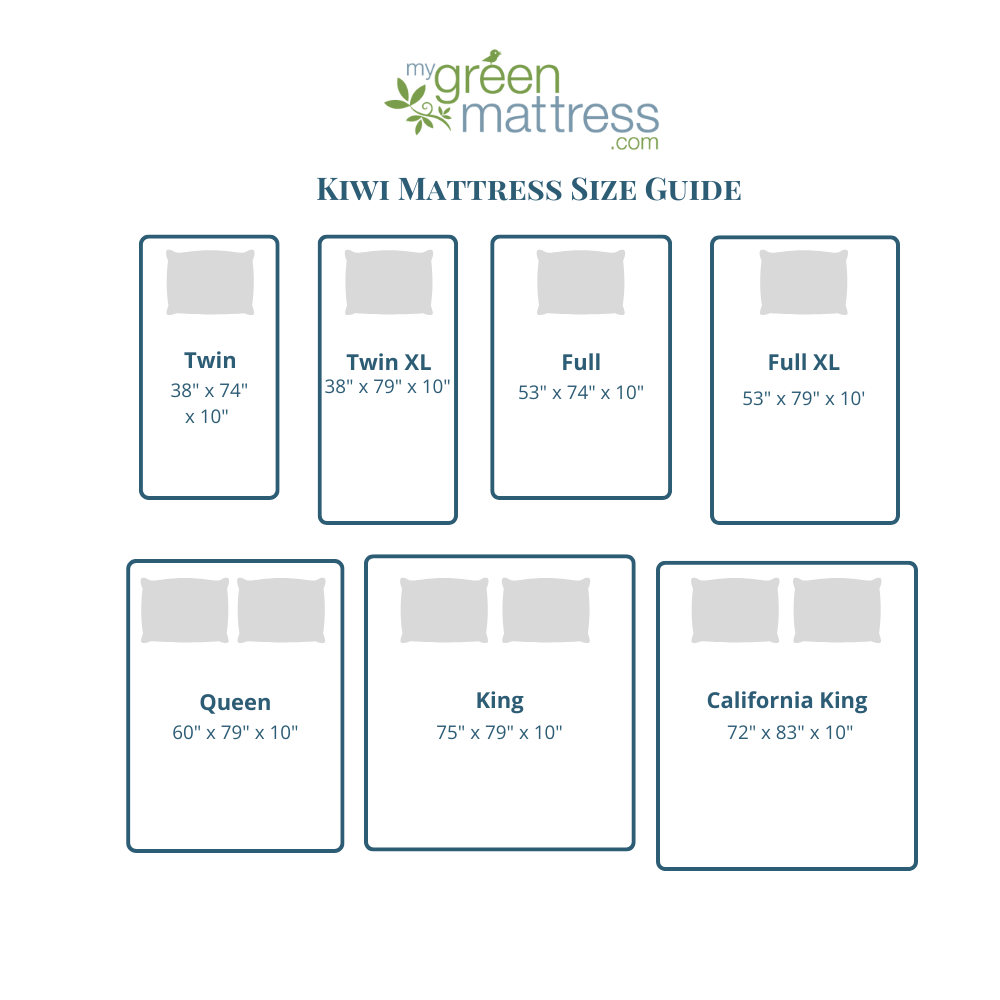
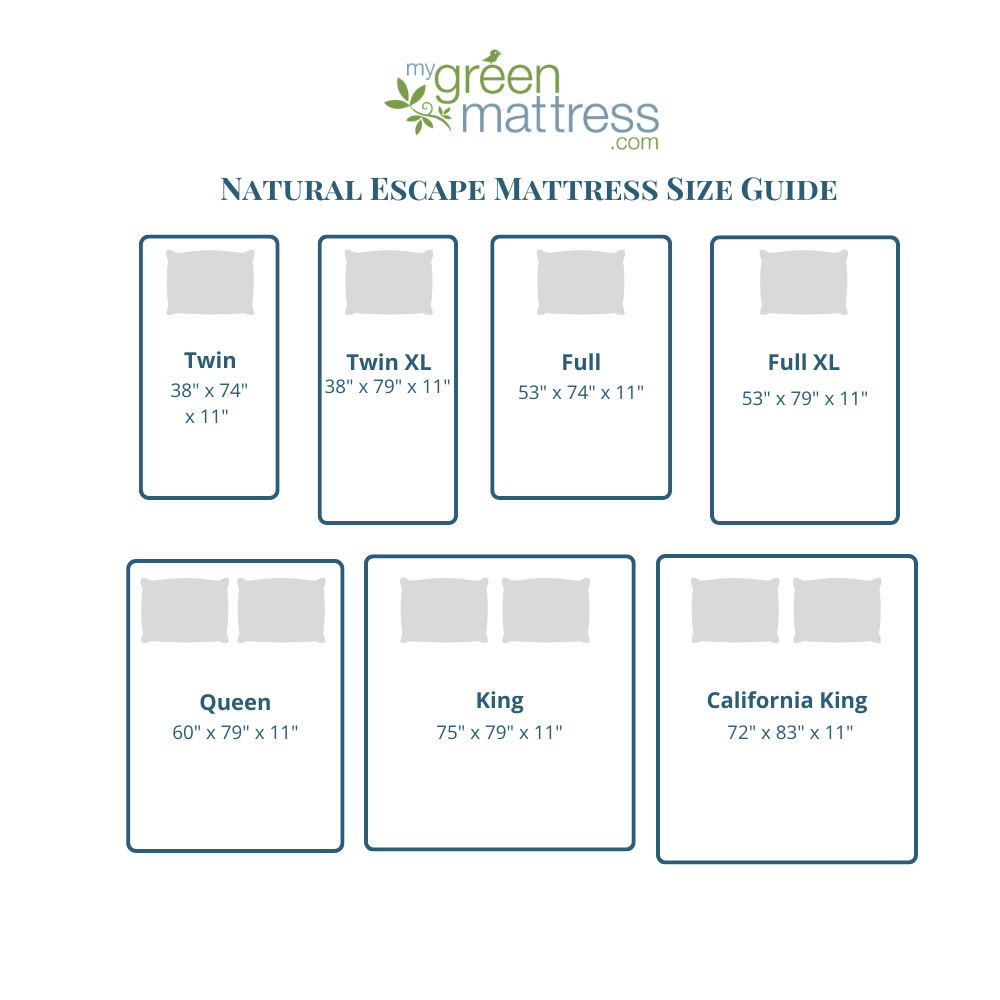
- A high quality bed. The more comfortable your mattress is, the more easily you’ll be able to get accurate home-based sleep study results. Learn what the healthiest type of mattress is today so you have one less health problem to worry about.
Who Can Benefit from a Sleep Study?
Considering a sleep study is often the result of one or more significant sleep-related health problems. Maybe you’ve been snoring or waking up extremely tired for years, or perhaps you’ve only recently struggled with rest. Either way, it’s prompted you to look at sleep studies and their benefits.
Anyone who’s currently experiencing a serious sleep-related issue can benefit from a sleep study. This includes families with babies experiencing sleep problems all the way up to seniors with sleep disorders.
What If I Can’t Sleep During a Sleep Study?
If you show up to your sleep study and discover that you can’t sleep, don’t worry. This is more common than you may think, especially because trying to fall asleep in a foreign environment is difficult.
If this happens, ask your sleep specialist or doctor if you can take a melatonin pill. This is a non-addictive substance that helps your brain recognize it’s time to sleep. You should fall asleep within 20 minutes of taking it.
Frequently Asked Questions About Sleep Studies
You can get pretty well prepared for a sleep study by reading about it, but nothing is comparable to going through with the event itself. The more you read about sleep studies, the more questions you probably have.
You can simplify your research journey by checking out the answers we’ve provided below. Check out these commonly asked questions about sleep studies:
What Do They Do During a Sleep Study?
During a sleep study, you can expect to have a few pieces of equipment placed on your body. This includes electrodes from an EEG, an effort belt for the respiratory rate measuring machine, and an oximeter for your left or right pointer finger.
Once the equipment is connected and you’re laying on the bed, lights will be dimmed as much as possible. Your doctor or sleep specialist running the sleep study will exit the room and go to the observation room.
From there, they’ll be watching data come in on your sleep monitors and ensuring the study is a success. They’ll also be available to address anything unexpected or to speak with you if you have a question in the middle of the study.
How Long Do You Need to Sleep for a Sleep Study?
In order for a sleep study to be successful, you need to sleep for about two hours and then be woken up. At that point, you’ll have a family member or friend driving you into the hospital or sleep center.
The reason you sleep a little bit and not for an entire night before the study is because your body needs to be “sleep-primed” for the rest of the study to run smoothly. When you’ve slept just a little, stay awake long enough to get to the hospital, and then fall asleep soon after, that’s when great things happen.
What Are Signs You Need a Sleep Study?
There are several adverse health indicators that make it clear a sleep study can be beneficial. Here are the most common ones:
- Waking up feeling exhausted (without any obvious causes, like staying up super late or drinking too much)
- Frequent sleep interruptions
- Feeling tired throughout the day, despite sleeping for seven to eight hours
- Irregular breathing or difficulty breathing, weather while asleep, awake, or both
- Constant or heavy snoring
- Frequent inability to fall and/or stay asleep
Can I Go to the Bathroom During a Sleep Study?
If you’re in the middle of a sleep study and you wake needing to use the restroom, simply ask your doctor or sleep specialist. Continuing the study despite a clear biological need is not something a doctor will force you to do.
Once you’re done using the restroom, keep yourself as relaxed and comfortable as possible. It will help you get back to sleep quickly and finish the study with as much continuity as you can.
Do People Watch You During a Sleep Study?
It might sound a bit strange, but yes, at least one professional will be observing you while you sleep during a sleep study. This is a necessary component of all third-party sleep studies in order to provide accurate results.
You may be wondering why the machines can’t capture all of the information needed for a sleep study. That’s a good question, and the fact is sleep equipment captures the majority of quantifiable data.
The reason a sleep specialist or doctor has to observe their patients while they’re sleeping is twofold. One, it’s the means by which to gather qualitative data, and two, it ensures the study is running smoothly. If there was an issue with the EEG but no one else was there, a sleep study could potentially run from the point of error to completion without collecting any data.
Want a mattress that will help you get the best sleep possible when you’re at home? My Green Mattress makes the highest quality certified organic hybrid mattresses in the world. Shop our products today for the rest you know you deserve.